

The Left is trying to destroy God’s ordained plan for family leadership, causing disdain for parental authority and reimagining culture to include more government control over the next generation.
![]() But you know that children—yours, your grandchildren, or even your neighbor’s children—are not political pawns to be won.
But you know that children—yours, your grandchildren, or even your neighbor’s children—are not political pawns to be won.
Thanks to the support of social conservatives like you, 2023 saw Family Policy Alliance (FPA) on the front lines of the fight to restore parental rights and Let Parents Parent.
 Our updated, comprehensive Back to School Guide is a valuable resource that’s educating parents about their rights and teaching social conservatives how to better protect children from the Left’s pro-abortion and LGBTQ agendas–agendas that continue to creep into our nation’s classrooms. Take advantage of the Back to School Guide and share it with a friend so that you, too, can champion the rights of parents in our schools.
Our updated, comprehensive Back to School Guide is a valuable resource that’s educating parents about their rights and teaching social conservatives how to better protect children from the Left’s pro-abortion and LGBTQ agendas–agendas that continue to creep into our nation’s classrooms. Take advantage of the Back to School Guide and share it with a friend so that you, too, can champion the rights of parents in our schools.
While schools are ground zero for the Left’s attacks, their plans to indoctrinate children go well beyond the classroom. Their messages often dominate on social media, through the judicial system, and even through sporting events. The ambush on our homes can feel overwhelming, but there is good news: Your generous support is allowing us to grow our defense of parental authority to be equally comprehensive.
After seeing how the Left used the judicial system to punish parents holding traditional sexual values, we drafted model legislation for 2024 that will protect parents from judicial activism in custody battles. Our Model Custody Protection Act seeks to prevent judges from favoring parents who affirm children’s transgender identities over those with traditional convictions about human sexuality.
Additionally, FPA has endorsed model legislation to implement age-verification requirements for children’s social media use. Social media has played no small part in conditioning our children to accept the Left’s agenda. The Protecting Kids Online Act simply seeks to restore parents’ control over their underage child’s online activity, including of the content they see.
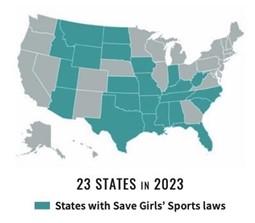 In 2023, FPA also helped five more states enact legislation to #SaveGirlsSports. The Left’s attempt to infiltrate athletics with their liberal agenda has far-reaching consequences for both the women athletes who are losing out and the next generation of children who are waiting to see if we will defend God’s design of men and women. Thanks to your support, more than 1.5 million female athletes–both at the high school and college level–won’t have to compete against men.
In 2023, FPA also helped five more states enact legislation to #SaveGirlsSports. The Left’s attempt to infiltrate athletics with their liberal agenda has far-reaching consequences for both the women athletes who are losing out and the next generation of children who are waiting to see if we will defend God’s design of men and women. Thanks to your support, more than 1.5 million female athletes–both at the high school and college level–won’t have to compete against men.
The fight to restore parental rights is far from over, and the Left never stops in seeking to claim ground that was never theirs to start with.
But we stand on solid ground.
We look forward to advancing reforms that restore parental authority in 2024, and with your help, we will continue to reclaim our homes one school board, one state, and one generation at a time.
May God bless your home now and in the new year,

Robert Noland
Director, Audience Engagement



